Am I doing too much? How much exercise can I do with Achilles tendonitis?
- Alison Gould
- 4 hours ago
- 7 min read
“Can I exercise with my Achilles tendinopathy?” is a question many of our patients ask. If you’ve been diagnosed with Achilles tendonitis/tendinopathy, one of the trickiest things to figure out is how much activity you should actually be doing.
Many people are told to “rest”, while others try to push through their symptoms and hope for the best. In reality, the sweet spot lies somewhere in between.
Remember, if you need help with an Achilles injury, you're welcome to consult one of our team via video call.

The terms tendinitis, tendonitis, tendinosis, and tendinopathy mean the same thing for all practical purposes, and we use these interchangeably in most of our articles.
In this article:
We've also made a video about this:
Using symptoms to judge activity levels
The right level of activity should allow you to stay active while still giving your Achilles tendon a chance to recover and become stronger. The challenge is learning how to judge when you’re doing too much, too little, or just enough.
Achilles tendinopathy often develops gradually. At first, you might only notice mild symptoms that don’t stop you from doing your usual activities. Over time, though, you might realise that you’re slowly having to cut back or modify what you do.
A common pattern is that the tendon feels reasonably good once you warm up and get moving, but then becomes stiff or sore later on – especially after sitting still or first thing in the morning. Some people also notice more discomfort when walking upstairs, downstairs, or on hills the following day.
The goal is not necessarily to have zero symptoms at all times. Instead, you want to keep symptoms at a low enough level that:
You can complete your normal daily activities without limping or compensating.
You can continue progressing your rehab exercises.
Your symptoms are not steadily worsening week after week.
How much pain is OK?
A useful way to monitor symptoms is with a simple pain scale out of 10.
0 to 3 out of 10: Generally acceptable.
4 to 6 out of 10: Warning sign that you might be overloading the tendon.
7 to 10 out of 10: Usually indicates that the tendon has been irritated too much.

For Achilles rehab, we tend to see better results by being a bit more conservative – we tend to advise patients to stay in that low “niggle only” range – roughly 0 to 2 out of 10. That means:
You might be aware of the injured area while doing an activity but would not class it as true discomfort or pain.
You can finish the activity without limping.
Your symptoms don’t dominate your attention afterwards.
You can still carry on with the rest of your day and the following day as normal.
Your rehab exercises are not negatively affected the next day.
💡 If you regularly find yourself unable to progress your strengthening exercises because your tendon is too sore from other activities, that’s often a sign that your overall activity level is currently too high.
Helping people with Achilles tendon injuries to find the right level of exercise and day-to-day activities for their current tendon strength and pain levels is something we do week in and week out via video call at Treat My Achilles. Find out more.
Comparing symptoms with the previous week
One of the easiest ways to judge whether you’re on the right track is to compare your symptoms from one week to the next.
Ask yourself:
Am I coping with the same level of activity more comfortably than last week?
Are my symptoms staying stable?
Am I gradually able to do more?
👍 If the answer is yes, you’re probably at a sensible activity level.
On the other hand, if your symptoms are gradually worsening or you’re able to do less and less over time, that usually means the tendon is being overloaded.
Comparing between activities
Different activities load the Achilles tendon in different ways. For example, you might feel fine after a gym session but noticeably stiffer after tennis or hill running. Or perhaps your tendon becomes more painful after a day with a very high step count at work.
It helps to compare:
Which activities flare your symptoms up most?
How do you feel over the following 24 hours?
Are high-step-count days more problematic?
Do long periods of sitting make stiffness worse?
This information can help you decide what needs modifying.
For example:
Replace hill sprints with flat running.
Swap some runs for cycling or swimming.
Choose lower-impact options in exercise classes.
Reduce long periods standing at work where possible.

Comparing recovery times
Another important clue is how long your symptoms take to settle after activity.
Early on, you might only feel mildly sore for a few hours. But if recovery starts taking several days, or each flare-up becomes more intense than the last, that’s usually a sign that your tendon is struggling to cope with the load.
For example:
A run used to irritate the tendon for one day, but now it takes three or four days to calm down.
Your pain used to peak at 2 out of 10, but now reaches 4 or 5 out of 10 after the same session.
👉 That’s often a sign that you need to reduce or adapt your activity levels temporarily.
How to adapt your activity levels
Reducing load does not necessarily mean stopping all activity.
Instead, think in terms of relative rest – modifying the activities that irritate your tendon most while still staying active overall.
Examples include:
Running on flat surfaces instead of hills.
Doing doubles tennis instead of singles.
Reducing session duration.
Mixing lower-impact intervals into classes.
Cross-training on a bike or cross-trainer.
Spreading physically demanding tasks across the week.
💡 The aim is to find a level your tendon can tolerate consistently while your strengthening programme gradually improves its capacity.
Keep an eye on function, not just pain
Sometimes pain improves, but if you look at what you've been doing, you notice a gradual decrease in activity – adjustments you made automatically without even noticing – e.g. you cannot give that final 20% that makes an all-out effort in hard exercise sessions.
You may notice that you’re:
Avoiding higher-intensity efforts.
No longer sprinting or jumping confidently.
Wearing supportive shoes constantly.
Modifying tasks around the house or garden without really thinking about it.
👉 These gradual changes are important warning signs. They often indicate that the tendon still lacks the full strength and resilience needed for your preferred activities.
Common training mistakes
Boom-and-bust cycles
“Boom-and-bust” is one of the most common patterns with Achilles tendinopathy.

Symptoms settle, so you suddenly return to normal activity levels with new enthusiasm, only for the tendon to flare badly again after a while. You then rest until things calm down, before repeating the cycle.
This indicates that your tendon isn’t quite ready yet for the level of activity you want to be doing. The problem is that rest alone doesn’t strengthen the tendon.
👍 A better approach would be to ensure, once the flare-up settles, that you structure your rehab and general training in such a way that it gradually builds the level of strength and endurance that matches what is needed for your goal.
Starting new activities too aggressively
A sudden increase in an activity that the tendon isn’t used to is a common trigger for tendon pain.
Maybe you start a new sport – let’s take padel, which is all the rage at the moment, as an example – and go from playing once a week to four times a week within a couple of weeks.. The tendon may cope initially, but after a few weeks, the symptoms start building because it’s just not been conditioned to handle this type of exercise load before.
👍 Tendons generally respond better to slow, steady progressions rather than rapid spikes in load.
Neglecting recovery days
Recovery days matter.
Your tendon needs time to adapt and grow stronger in reaction to the stress you place on it. Without adequate recovery between sessions or general activities that load it, the tendon may struggle to keep up with the repeated demands being placed on it.
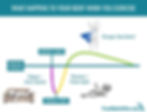
👍 For many people, having at least one or two lower-load days each week is helpful.
That doesn’t necessarily mean doing nothing. It might simply mean:
Lower step counts
Less time on your feet
Avoiding high-impact loading, e.g. use the cross-trainer rather than go running
Scaling back calf-heavy activities on that day.
The 80/20 rule
It can also help to look at the intensity balance of your weekly exercise.
A useful guideline is:
Around 80% of activity at an easy-to-moderate intensity
Around 20% at higher intensity.
Easy-to-moderate exercise should still allow you to comfortably hold a conversation, while hard efforts leave you noticeably short of breath.
👉 If too much of your week sits in the high-intensity category, your tendon might not be getting enough recovery.
Preparing for an important event
If you have an active holiday, tournament, or race coming up, planning ahead becomes especially important.
Rather than suddenly increasing activity shortly beforehand, try to gradually build towards the demands of the event over weeks or months.

Useful strategies include:
Progressing your strengthening exercises steadily
Gradually increasing the volume of the activity you will be doing
Including recovery days
Reducing training load slightly in the week before the event
Temporarily reducing rehab intensity afterwards if needed.
Some people also find it useful to use “deload” weeks – for example, building activity for three or four weeks, then having a lighter week before progressing again.
A gradual increase of around 10% per week in overall activity volume is often a sensible approach.
How we can help
Need help with your Achilles or related injury? You’re welcome to consult one of the team at TMA online via video call for an assessment of your injury and a tailored treatment plan.
We're all UK Chartered Physiotherapists with Master’s Degrees related to Sports & Exercise Medicine or at least 10 years' experience in the field. All of us have a wealth of experience working with athletes across a broad variety of sports and ranging from recreationally active people to professional athletes. You can meet the team here.

About the author
Alison Gould is a chartered physiotherapist and holds an MSc in Sports and Exercise Medicine. You can follow her on LinkedIn, Facebook, Instagram, and Twitter.












